Patients with malignant haematological diseases may present with dramatic and life-threatening complications. General physicians must be able to recognise these conditions as prompt treatment can be life-saving. Hyperleukocytosis and leukostasis and febrile neutropaenia in patients with haematologic malignancies are two such conditions highlighted in this article.
HYPERLEUKOCYTOSIS AND LEUKOSTASIS IN HAEMATOLOGIC MALIGNANCIES
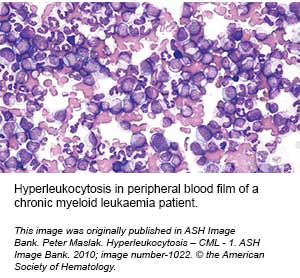 Hyperleukocytosis has been variably defined as a total white cell count (WBC) of 50 x 109/L or 100 x 109/L. Leukostasis is a medical emergency characterised by hyperleukocytosis and symptoms of tissue hypoperfusion. It is most commonly seen in patients with acute myeloid leukaemia (AML) or chronic myeloid leukaemia (CML) in blast crisis.
Hyperleukocytosis has been variably defined as a total white cell count (WBC) of 50 x 109/L or 100 x 109/L. Leukostasis is a medical emergency characterised by hyperleukocytosis and symptoms of tissue hypoperfusion. It is most commonly seen in patients with acute myeloid leukaemia (AML) or chronic myeloid leukaemia (CML) in blast crisis.
Symptoms of leukostasis occur less frequently in patients with acute lymphoblastic leukaemia (ALL) or chronic lymphocytic leukaemia (CLL) unless the WBC exceeds 150 x 109/L.
Pathologically, it is characterised by intravascular accumulation of blasts in the microvasculature, resulting in increased blood viscosity and decreased perfusion. It is also postulated that local hypoxaemia may be exacerbated by the high metabolic activity of the dividing blasts and release of cytokines.
SIGNS AND SYMPTOMS
Clinically, this should be suspected when the full blood count (FBC) shows hyperleukocytosis in a patient presenting with respiratory or neurologic distress. Patients can present with dyspnoea and hypoxia which can be picked up on pulse oximetry. Neurologic signs and symptoms include visual changes, headache, dizziness, change in mental state and unsteadiness in gait. There is also increased risk of intracranial haemorrhage.
Besides affecting the central nervous system, eyes and lungs, other manifestations include myocardial ischaemia, limb ischaemia or bowel infarction. Leukostasis may also occur where the clinical picture is less typical and at a WBC lower than the arbitrarily defined figures, especially in rapidly increasing blasts counts.
INVESTIGATIONS
Besides elevated WBC and blasts in the FBC, evidence of tumour lysis syndrome (TLS) may be present in up to 10% of patients with leukostasis. These include raised creatinine, hyperuricaemia, hyperkalaemia, hyperphosphatemia and hypocalcaemia. Disseminated intravascular coagulation (DIC) may manifest with thrombocytopaenia and an abnormal coagulation profile.
MANAGEMENT
The diagnosis requires a high degree of suspicion. It is made clinically when a patient presents with a high white cell count and symptoms suggestive of tissue hypoxia.
Leukostasis constitutes a medical emergency. Prompt treatment is indicated. If left untreated, the one-week mortality can be as high as 40%. Symptomatic patients have a worse prognosis when compared to asymptomatic patients with hyperleukocytosis alone.
The patient should be urgently referred to the Emergency Department of a hospital, where he should be rapidly stabilised. Rapid cytoreduction can be achieved with chemotherapy or leukapheresis. This should be accompanied by tumour lysis syndrome prophylaxis and aggressive hydration and allopurinol. Specialised, supportive care such as mechanical ventilation for respiratory failure may be required.
FEBRILE NEUTROPAENIA IN PATIENTS WITH HAEMATOLOGIC MALIGNANCIES
Febrile neutropaenia (FN) is one of the most serious adverse events in patients with haematologic malignancies treated with chemotherapy. Since the magnitude of the inflammatory response may be muted in the neutropaenic patients, a fever may be the earliest and only sign of infection. Infections in these patients can progress rapidly, leading to life-threatening complications.
FN is considered a medical emergency. Prompt initiation of broadspectrum antibiotics is necessary to avoid progression to sepsis and possibly death.
DEFINITIONS
The Infectious Diseases Society of America (IDSA) defines fever in neutropaenic patients as a single oral temperature of >38.3˚C (101˚F) or a temperature of >38.0˚C (100.4˚F) sustained for >1 hour.
Neutropaenia is an absolute neutrophil count (ANC) <1500 cells/μL, and severe neutropaenia is defined as ANC <500 cells/μL or that is expected to decrease below 500 cells/μL during the next 48 hours, and profound neutropaenia is an ANC <100 cells/μL. The risk of clinically important infections rises as the ANC decreases.
Initial neutropaenic fever syndromes can be classified into 3 categories:
- Microbiologically documented infection – neutropaenic fever with a clinical focus of infection and an associated pathogen
- Clinically documented infection – neutropaenic fever with a clinical focus (e.g. pneumonia) but without the isolation of an associated pathogen
- Unexplained fever – neutropaenic fever with neither a clinical focus of infection nor an identified pathogen
RISM OF COMPLICATIONS
The IDSA guideline considers low-risk patients as those who are expected to be neutropaenic (ANC <500 cells/ μL) for ≤7 days and those who have no active comorbidities or evidence of significant hepatic or renal dysfunction.
High-risk patients are those who are expected to be neutropaenic (ANC <500 cells/μL) for >7 days. Patients with neutropaenic fever who have ongoing comorbidities or evidence of significant hepatic or renal dysfunction are also considered to be high-risk, regardless of the neutropaenia duration.
Assessment of the risk of complications is crucial in patients with neutropaenic fever as this will dictate the approach to therapy, such as the need for inpatient admission and intravenous antibiotics.
PATHOGENESIS
 Chemotherapy-induced mucositis and seeding of the bloodstream from endogenous flora in the gastrointestinal tract is believed to cause the majority of neutropaenic fevers. Immune defects related to the underlying haematologic malignancy and the immunosuppressive effects of chemotherapy are other contributory factors to the pathogenesis of neutropaenic fever.
Chemotherapy-induced mucositis and seeding of the bloodstream from endogenous flora in the gastrointestinal tract is believed to cause the majority of neutropaenic fevers. Immune defects related to the underlying haematologic malignancy and the immunosuppressive effects of chemotherapy are other contributory factors to the pathogenesis of neutropaenic fever.
An infectious source is identifiable in approximately 20-30% of febrile neutropaenic episodes.
About 80% of identified infections arise from the patient’s endogenous flora. Gram-positive bacteria (e.g. Staphylococcus aureus, Enterococcus spp, Streptococcus pneumonia) are the most common causes of infections in the febrile neutropaenic patients.
However, infections caused by gramnegative bacteria (e.g. Pseudomonas aeruginosa, Klebsiella spp, Escherichia coli) are associated with most serious consequences.
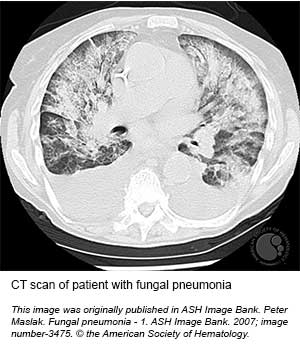
Invasive fungal infections are more common in high-risk patients with prolonged fever syndromes, with Candida and Aspergillus spp accounting for most of these infections.
Viral infections, including infections caused by respiratory viruses and human herpes viruses, are also more common in high-risk patients with neutropaenia.
MANAGEMENT
It is critical to recognise neutropaenic fever early and for empiric broad-spectrum antibiotics to be initiated promptly to avoid progression to a sepsis syndrome and possible demise.
The managing oncologist can educate and instruct the patient and their caregivers to recognise symptoms that require prompt medical attention and to inform healthcare providers on their chemotherapy administration.
These patients should be assessed without delay and referred to a hospital where empiric broad-spectrum antibiotics can be initiated immediately after blood cultures have been obtained. International guidelines advocate the administration of empiric antibiotics within 60 minutes of presentation in all patients with febrile neutropaenia. Empiric therapy aims to cover the most likely pathogens that may rapidly cause serious or life-threatening infections in neutropaenic patients.
GPs can call for appointments through the GP Appointment Hotlines at
6321 4402 (SGH) or
6436 8288 (NCCS).
By: Adj Assoc Prof Wong Gee Chuan, Senior Consultant, Department of Haematology, Singapore General Hospital; SingHealth Duke-NUS Blood Cancer Centre
Dr Wong Gee Chuan is a Senior Consultant in the Department of Haematology, Singapore General Hospital and also Adjunct Associate Professor, Yong Loo Lin School of Medicine, National University Singapore and Adjunct Assistant Professor, Duke-NUS Medical School. Her interest is in Acute Leukaemias.
Trained in the MD Anderson Cancer Center, Houston, Texas, Dr Wong spearheaded the setup of the Leukaemia Registry and the Myeloproliferative Disorders Registry in the Department of Haematology, Singapore General Hospital. She also developed Leukaemia protocols, antibiotics and antifungal guidelines for immunocompromised hosts.
Besides authoring patient guidebooks on Leukaemia, Lymphoma and Febrile Neutropaenia, she has also published extensively on Malignant Haematology and Myeloproliferative Disorders and conducted multiple trials in these areas. She is the Director, Acute Leukaemia Service, Department of Haematology, Singapore General Hospital. Her current research interests include treatment of acute leukaemia and management of febrile neutropaenia in immunocompromised hosts. She also has specialist accreditation in Palliative Medicine.
REFERENCES
Hyperleukocytosis and Leukostasis in Haematologic Malignancies
1. Porcu P, Cripe LD, Ng EW et al. Hyperleukocytic leukemias and leukostasis: a review of pathophysiology, clinical presentation and management. Leuk Lymphoma 2000; 39:1
2. Lester TJ, Johnson JW, Cuttner J. Pulmonary leukostasis as the single worst prognostic factor in patients with acute myelocytic leukemia and hyperleukocytosis. Am J Med 1985; 79:43
3. Azoulay E, Fieux F, Moreau D et al. Acute monocytic leukemia presenting as acute respiratory failure. Am J Respir Crit Care Med 2003; 167:1329
4. Porcu P, Farag S, Marcucci G et al. Leukocytoreduction for acute leukemia. Ther Apher 2002; 6:1
Febrile Neutropaenia in Patients with Haematologic Malignancies
1. Freifeld AG, Bow EJ, Sepkowitz KA et al. Clinical practice guideline for the use of antimicrobial agents in neutropenic patients with cancer: 2010 update by the Infectious Diseases Society of America. Clin Infect Dis 2011; 52:e56
2. Flowers CR, Seidenfeld J, Bow EJ et al. Antimicrobial prophylaxis and outpatient management of fever and neutropenia in adults treated for malignancy. American Society of Clinical Oncology clinical practice guideline. J Clin Oncol 2013; 31: 794
3. From the Immunocompromised Host Society. The design, analysis and reporting of clinical trials on the empirical antibiotic management of the neutropenic patient. Report of a consensus panel. J Infect Dis 1990; 161:397
4. Dellinger RP, Levy MM, Carlet JM et al. Surviving Sepsis Campaign: international guidelines for management of severe sepsis and septic shock: 2008. Crit Care Med 2008; 36:296
