General practitioners are the essential link to managing diabetes in the community. Read about the important role you can play in helping Muslim diabetic patients navigate the challenges faced in their diabetic management during the fasting month.
RAMADAN FASTING
Ramadan fasting is an annual month-long consecutive-day fasting performed as one of the five pillars of Islam.
Whilst it is a religious obligation for adult healthy Muslims, there are exemptions and alternative practices when faced with health challenges to fasting safely, both acutely or in the longer term, including for people with diabetes mellitus (DM).
In Singapore, the duration of fasting is fixed at approximately 14 hours daily for 29 or 30 consecutive days annually, according to the Muslim calendar. In the month of Ramadan, there are changes in daily routines, with extended periods between meals due to an earlier morning meal before dawn (Sahur) and a later evening meal at sunset (Iftar).
Whilst locally, daytime physical activity may not differ much, there is an average of a twofold increase in supplementary prayers performed at night, due to the attraction of increased spiritual rewards when performed in the month. With the increased number of night-time prayers, sleep patterns are altered and sleep durations are reduced.
PREVALENCE OF DIABETES AMONG SINGAPORE MUSLIMS
The latest National Population Health Survey 2019 reported the prevalence of diabetes amongst Malays at 14.4%, compared to Indians at 14.2% and Chinese at 8.2%.
Considering that the General Household Survey 2015 reported that 99.2% of Malays and 21.3% of Indians make up most of the Muslim population in Singapore, which is 14% of the resident population, this accounts for a substantial proportion of people with diabetes potentially undergoing Ramadan fasting year by year.
THE IMPACT OF RAMADAM FASTING ON PEOPLE WITH DIABETES
Abstaining from food and fluid intake during fasting hours poses challenges for Muslims with comorbidities.
It was previously reported that people with diabetes were found to have:
A multifold increased risk of acute diabetes complications without adequate preparation for Ramadan fasting
A daily glucose trend showing increased hypoglycaemia during fasting hours
Increased hyperglycaemia during eating hours
Whilst the duration of fasting remains constant from year to year in Singapore, the altered meal patterns and circadian rhythms with differing sleeping durations and potentially varying levels of physical activity necessitate dietary and treatment adjustments to sustain good control for diabetes, even in those with previously uneventful experiences during Ramadan.
As such, a yearly pre-Ramadan reassessment can provide the latest risk assessment, as this chronic condition may change each year with chronic complications setting in.
Patient background In Singapore, a large proportion of people with diabetes are being managed by primary care. Similarly, Mdm A has been managed by her primary care doctor for the last 20 years since diagnosis. At 64 years old now, she has moved in with her daughter to be involved in the care of her grandchildren. She has also minimised her clinic visits during the COVID-19 pandemic, opting to self-medicate and relying on medication deliveries for diabetes, hypertension and hyperlipidaemia when they run out, due to fear of exposure after she caught the COVID-19 infection earlier in the year. Diabetes screening results During her first visit to the nearby general practitioner (GP) clinic, she underwent the annual diabetes screening and investigations. Her glycaemic control showed a glycated haemoglobin level (HbA1c) of 10.5% which is markedly raised compared to her previous screening six to 12 months ago, with levels ranging between 7% to 7.3%. Mdm A is on basal insulin twice daily, with subcutaneous Levemir 24 units pre-breakfast and 10 units at bedtime (total daily dose insulin 0.51 units per kg body weight per day), with episodes of hypoglycaemia during her regular twice weekly fasting. This was discovered when her astute GP initiated her on self-monitoring of capillary blood glucose. 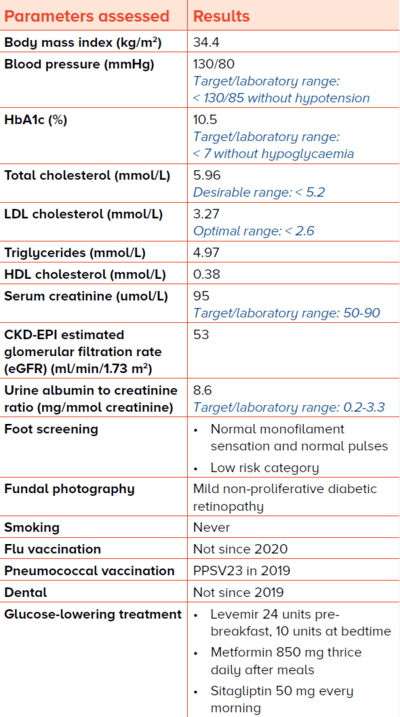 Table 1 Baseline screening results |
HOW GPs CAN MANAGE DIABETES WITH RAMADAN FASTING
Pre-Ramadan preparation and risk calculation
With pre-Ramadan preparation2, studies have shown that the risk of acute diabetes complications is reduced with consequent safer fasting during Ramadan, and improved self-care with resultant sustained improvement in glycaemic control.
Hence, international experts recommend that people with diabetes are assessed with risk stratification pre-Ramadan in the latest guidelines1.
Patient education and management
It is crucial for patients to make an informed decision on whether to fast. In order to reduce the risk of complications, it is also important to optimise their glycaemic control, focus on education and provide appropriate treatment adjustments with close monitoring and patient empowerment.2
This can be performed at the primary care level where patients can have easy access to their GP clinic.
WHEN TO REFER TO A SPECIALIST
For patients who are at moderate or high risk of complications during fasting, it is recommended to refer them to the specialist clinic to undertake the pre-Ramadan preparation at least two to three months before Ramadan starts.
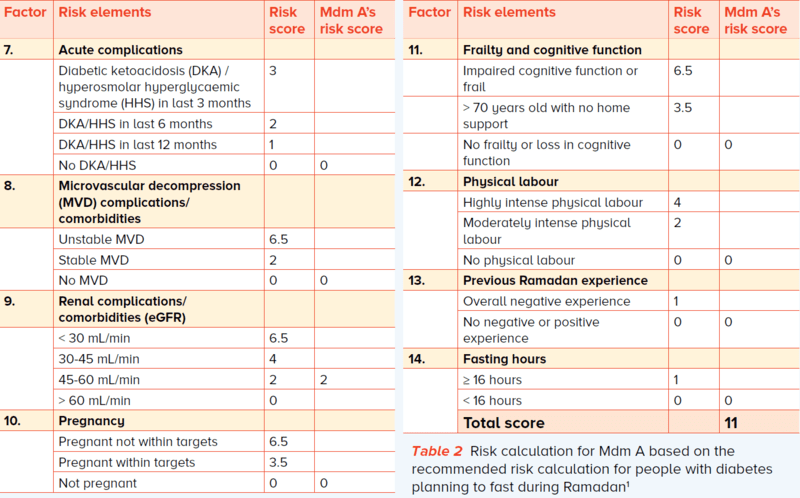
Risk calculation Mdm A’s GP performed her risk calculation. Her risk score was 11 (Table 2) which puts her in the high risk level for fasting. 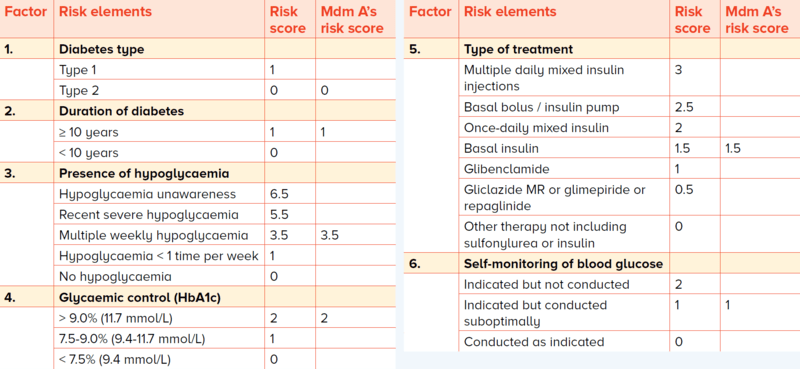
Recommendation for specialist referral After discussing with Mdm A and noting her insistence on fasting, in view of the concern regarding her fasting without guidance and to reduce her risk of acute complications as well as improve her overall glycaemic control and control of comorbidities, she was referred to Sengkang General Hospital. An appointment was booked at the Diabetes and Ramadan Clinic for the Diabetes Education and Medication Adjustment in Ramadan (DEAR) programme3.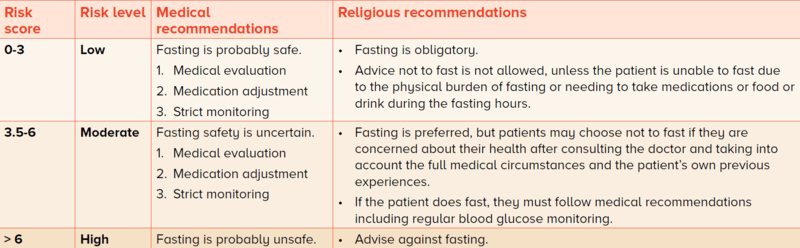 
Table 3 Risk score, risk categories and medical and religious recommendations for fasting1 |
THE DIABETES EDUCATION AND MEDICATION ADJUSTMENT IN RAMADAN (DEAR) PROGRAMME
The DEAR programme is an outpatient service consisting of clinics, education sessions and remote monitoring by a diabetes care team consisting of specialist nurses and allied health professionals.

Figure 1 DEAR programme for Ramadan fasting
Patient education
A local survey had previously shown that there is a diabetes knowledge-to-practice gap relevant to Ramadan4. Hence, revisiting general diabetes education followed by providing pre-Ramadan education is of essence.
The general education should be provided annually, revising the diabetes skill sets such as understanding medications, treatment of complications, keeping physically active, healthy meal planning and coping skills with the support of a dietitian, physiotherapist, psychologist, medical social worker and when needed, a pharmacist.
Ramadan-focused education
Focused education (Figure 2) is performed by a multidisciplinary team and provided after ensuring general diabetes education and general diabetes management is optimised.
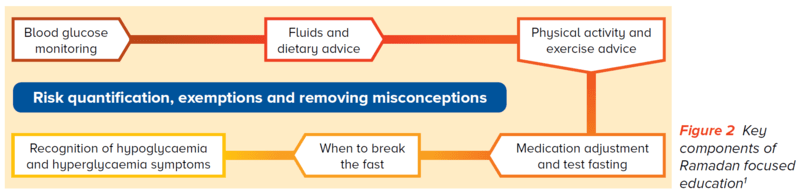
The DEAR programme also consists of pre-Ramadan assessment for risk stratification, optimisation of glycaemic control and the reduction of risks of complications through adjustment of the treatment regimen, test fasting and glucose monitoring.
Continued follow-up and monitoring
This is followed by feedback through remote glucose monitoring or if needed, further consultations to optimise and reduce risks further. The experience of patients fasting is reviewed after the fasting period.
Benefits of the DEAR programme
The DEAR programme is an outpatient service that was launched in 2016. Our study of moderate- to high-risk patients in this programme at the specialist outpatient clinic showed improvement in acute diabetes complications for both hypoglycaemia and hyperglycaemia with sustained improvement in glycemic control3. This is likely related to improved glycaemic control and skill sets through self-empowerment.
Pre-Ramadan assessment and management The discussion of Mdm A’s plans to fast was again revisited, and she was advised not to. However, her diabetes care team concurrently worked with her to manage her risk of diabetes complications, should she decide to proceed with fasting. She was assessed to have irregular insulin administration, poor understanding of diabetes and her treatment, as well as poor matching of insulin to her meals despite a total daily dose of insulin of 0.5 units/kg/day. She was initiated on a basal bolus insulin regimen to target each component. Empagliflozin was also added on. 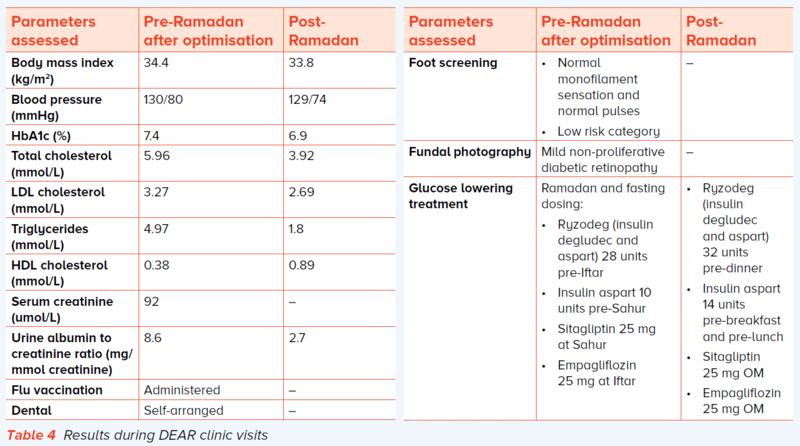
Management during Ramadan fasting She was started on insulin coformulation due to her larger meals at dinner and during sunset meals (Iftar), with better glycaemic control and less hypoglycaemia during test fasting through feedback of glucose readings. She had better glucose control with reduced amplitude of her glucose swings to acceptable targets with capillary glucose levels ranging between six to ten mmol/L. Her risk level was reduced to moderate risk. During remote glucose feedback when performing Ramadan fasting, no episodes of hypoglycaemia were found during capillary and flash glucose monitoring. She was able to cope with further weekly fasting after Ramadan with no further episodes of hypoglycaemia. Post-Ramadan shared care with GP She was reviewed post-Ramadan with improved glycaemic control without hypoglycaemia and some weight loss. This may concur with previous local data suggesting that improved glycaemia is related to reduced body fat mass and reduced visceral adiposity in females5. Her care was transferred back to her GP through the GP Partners programme to enable fast track referrals and support for special circumstances such as Ramadan fasting6. |
THE GP’S ROLE IN DIABETES MANAGEMENT FOR RAMADAN FASTING
A large proportion of people with diabetes are managed in primary care and are likely to be able to fast safely if they are of low risk.
GPs are the essential link as the first line in the care of people of diabetes in the community. Early referral of patients who are deemed moderate to high risk but planning to fast enables better preparation of these patients to understand their risk and improve self-care during the challenging period.
Thereafter, shared care with GPs as the first line will complete the puzzle in the comprehensive care of the diabetes patient.
CONCLUSION
Ramadan fasting may be challenging for people with diabetes. Pre-Ramadan assessment to optimise glycaemic control and promote self-care, coupled with easy access to primary care providers for necessary intervention to avert complications, is of essence. Specialist care provides a multidisciplinary team necessary to prepare and support those at moderate to high risk to undergo fasting more safely.
REFERENCES
Hassanein M, Afandi B, Yakoob Ahmedani M et al. Diabetes and Ramadan: Practical guidelines 2021. Diabetes Res Clin Pract. 2022 Mar;185:109185. doi: 10.1016/j.diabres.2021.109185. Epub 2022 Jan 8. PMID: 35016991.
Zainudin SB, Yeoh ECK. Preparing Muslims with Diabetes for Ramadan Fasting in Singapore – A Clinical Approach and Review of Current Practice. Singapore Med Journal 2021, 1-22 https://doi.org/10.11622/smedj.2021047
Zainudin SB, Abu Bakar KNB, Abdullah SB, Hussain AB. Diabetes education and medication adjustment in Ramadan program prepares for selfmanagement during fasting with tele-health support from pre-Ramadan to post-Ramadan. Ther Adv Endocrinol Metab. 2018 Jun 12;9(8):231-240. Doi: 10.1177/2042018818781669. JIF: 3.978.
Zainudin SB, Ang DY, Soh AWE. Knowledge of diabetes and safe practices during Ramadan fasting among Muslim patients with diabetes in Singapore. Singapore Med J. 2017 May:58(5):246-252. Doi: 10.11622/smedj.2016085. JIF:1.081
Yeoh ECK, Zainudin SB, Loh WN et al. Fasting during Ramadan and Associated Changes in Glycaemia, Caloric Intake and Body Composition with Gender Differences in Singapore. Ann Acad Med Singapore. 2015 Jun;44(6):202-206. JIF:1.041
Zainudin SB, Hussain AB. The current state of knowledge, perception and practice in diabetes management during fasting in Ramadan by healthcare professionals. Diabetes Metab Syndr. 2018 May;12(3):337-342. Doi: 10.1016/j.dsx.2017.12.025.
Dr Sueziani Zainudin is an Endocrinologist at Sengkang General Hospital. She has a keen interest in diabetes mellitus and Ramadan fasting. She works closely with the international expert alliance with authorship of its latest international guidelines.
She plays an active role in the education, research and clinical care regarding fasting during Ramadan including healthcare professional education through close networking with the alliance.
GPs can call the SingHealth Duke-NUS Diabetes Centre for appointments at the following hotlines:
Singapore General Hospital: 6326 6060
Changi General Hospital: 6788 3003
Sengkang General Hospital: 6930 6000
KK Women's and Children's Hospital: 6692 2984
Singapore National Eye Centre: 6322 9399
Tags:
;
;
;
;
News Article;
SingHealth Duke-NUS Diabetes Centre;
SingHealth Duke-NUS Diabetes Centre;
Article;
Defining Med;
;
;
;
;
Defining Med;Patient Care;Medical News (SingHealth)
